Acute Shoulder Tendonitis (calcific)
Taking my advice is entirely at your own risk
but there is nothing that is medically contentious about what I am suggesting.
PDF DOWNLOAD
About Michael Kurer FRCS FRCS(Orth) Consultant Orthopaedic and Shoulder Surgeon
I have been a shoulder surgeon for 25 years and there is a rare but very treatable condition that patients and doctors need to know about. It is the Worst Shoulder Pain I know. That is why I have created this website. This is for advice.
Acute Shoulder Tendonitis (calcific)
It is rare but very typical and thus easy to diagnose, once you know about it. It is also very easy to treat.
Your History
This history is typical. Men and women between the ages of 30 and 50 will suffer from it and it comes out of the blue for no reason. Over hours or days, the patient will notice the onset of very very sharp pain in the shoulder, usually at the front corner. Any attempt to move the shoulder causes terrible extra pain and the patient can’t do it. They try to think of something that might have brought it on but they can’t. The pain then gets worse and worse over a day or two and they don’t know what to do. Even when travelling in a car, the bumps are enough to provoke the pain. The patient is otherwise well with no temperature.
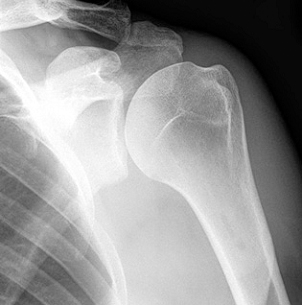
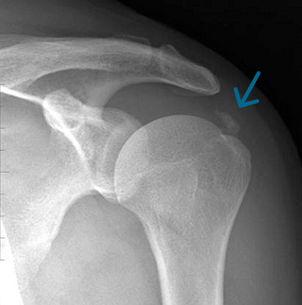
The pain is such that they usually go to the doctor or more often the hospital Emergency Department and are seen by a junior doctor or nurse practitioner who accepts that the shoulder is very painful and also doesn’t know why. An x-ray is arranged, which sometimes shows some calcification in a tendon. The x-ray is otherwise normal.
The practitioner then usually offers some analgaesics and anti-inflammatory tablets, which may have already been tried but may take the edge off the pain. A diagnosis of ‘rotator cuff pain’ is made but no one knows what else to do, although it will settle down in a few weeks.
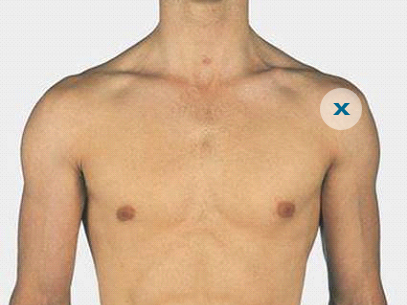
Examination
Now actually, when one examines the shoulder carefully, there is usually one spot, where even light finger pressure provokes extra pain. It is the epicentre of what is happening. It is again, usually at the front corner and any repeated light touch pressure on that point, really hurts.
What is the Diagnosis
I call this condition ‘Acute Tendonitis (Calcific)’ because it is an acute inflammation of the tendon which is part of a muscle which normally lifts the arm. Trying to lift, using that muscle provokes so much pain from the tendon, that the patient has to stop. I call it ‘calcific’ because quite a few of these patients already have some calcium visible on the x-ray, which is a chronic, long-standing calcification they usually don’t know about, suggesting a tendency to concentrate calcium salts (like chalk) in the tendon there.
My explanation is that this is a new fresh attack of acute calcium, invisible on x-ray, which is like having acid poured into the tendon.
Many show no calcification on the x-ray.
My Treatment
I am pleased to say that there is a very simple treatment. That is to inject cortisone towards (though not necessarily into) the tender spot!
One does not need ultrasound scan nor an MRI scan nor an ultrasound guided injection.
Injection Technique
I inject cortisone (triamcinolone 40mg) and lidocaine 1% (or bupivacaine 0.5%) 3mls into that area. It really is just a trigger point injection.
I inject through the skin and 1cm deeper, through the deltoid muscle, so only 1.5 cm. One does not have to ‘hit the tendon, or bone, or any calcification’.
(Provided there is no contraindication such as gastric or renal problems, I have also added either injectable diclofenac 50 mg or ketorolac 30 mg to the mixture, hoping that would have an effect before the cortisone kicks in later.)
I reiterate, the needle does not need to go into the tendon as such. The cortisone and local anaesthetic just need to wash over the surface of the tendon. One then waits 5 minutes to see if the local anaesthetic effect has dulled the pain, which means that the cortisone which is mixed with the lidocaine, (and NSAID if used), is also touching the inflamed area. The area of most tenderness should now be much less tender to the touch. If so, that’s it. Job done!
If there is more than one very tender area, or if the first injection hasn’t ‘hit the spot’, then one repeats the injection process until the tender spot is much less tender.
Then the patient simply has to wait 2-3 days. The arm is rested in a sling or on a cushion. Then the pain will dramatically improve and they will be able to start to use the arm again. There will be some minor ache but local professionals will be able to deal with that in conventional ways. The shoulder will not become stiff.
I have never known a patient to get this twice, although it can occur in the other shoulder but then they know what to do immediately to get it treated.

Other Comments
You will find that calfcific tendonitis is described in the literature, usually in chronic form. That is not this. Doctors are good at treating it. You may find acute calcific tendonitis reported, with suggestions such as putting needles into the calcium under x-ray control and trying to suck out the calcium. This is very hard to arrange and is quite unnecessary. You may find reports of washing the shoulder out under anaesthetic as part of an arthroscopy. Again, it is quite unnecessary for the acute attack and not usually necessary in chronic pain.
Important Negatives
Another painful condition is ‘frozen shoulder’ but that takes weeks and months to build up and is usually associated with profound stiffness. It tends to occur in patients over 40 or 45. Of course an injury will hurt the shoulder but there is no injury here. Patients may overdo it at the gym but that causes an aching and not this knife-like pain for no reason, that one gets in these cases.
I hereby also provide a pdf version of this website, which you can print out and show to a doctor whom you think can help you.